IN THIS LESSON
Coronary Artery Disease
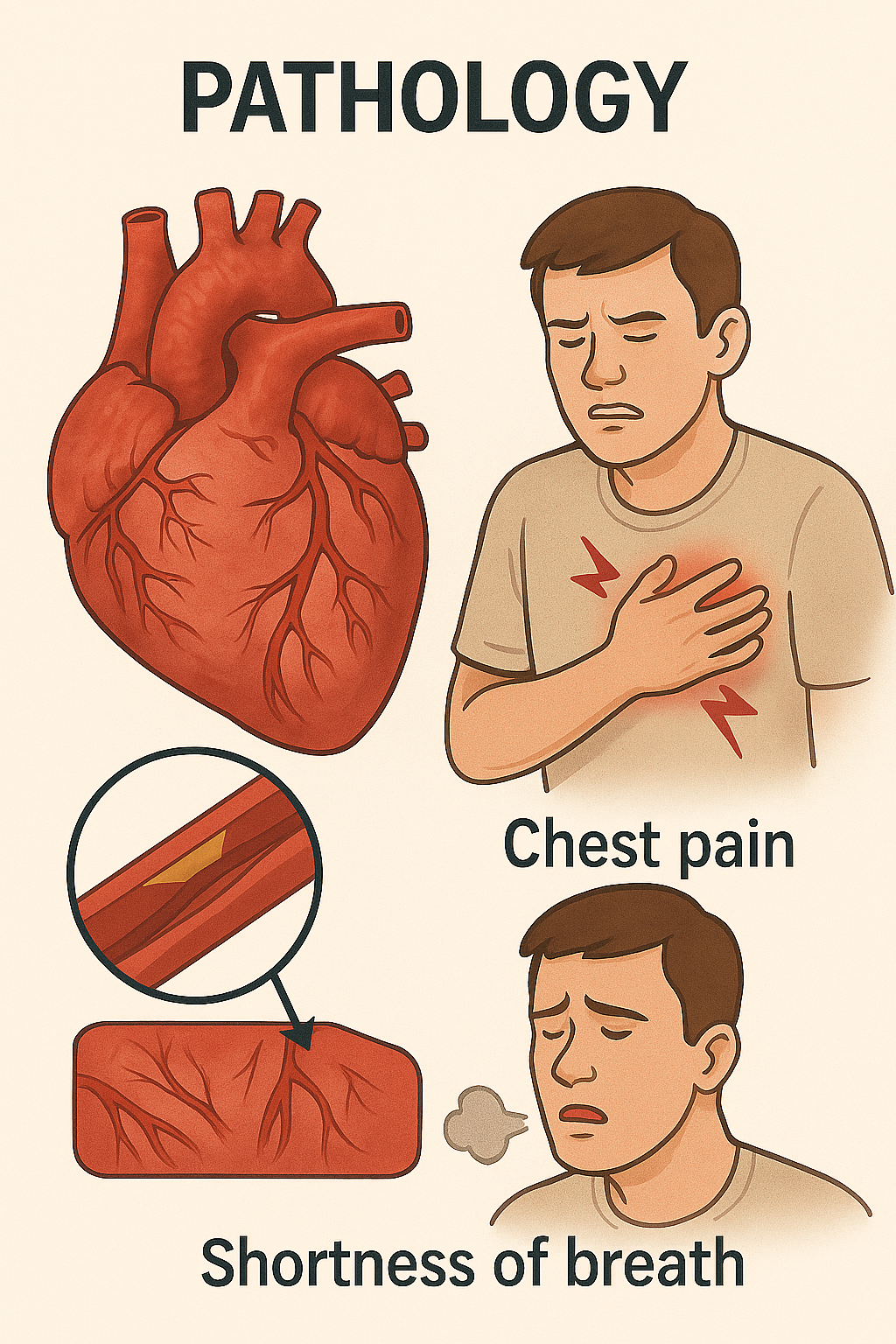
Pathophysiology:
Caused by atherosclerosis—buildup of lipid plaques in coronary arteries → narrowing of the vessel lumen → reduced blood flow to myocardium.
Leads to myocardial ischemia, especially during exertion when oxygen demand increases.
Plaque rupture may cause thrombosis, resulting in acute coronary syndromes (unstable angina, MI).
Clinical Features:
Angina pectoris: pressure-like substernal chest pain radiating to left arm, neck, or jaw.
Dyspnea, diaphoresis, nausea, fatigue, or syncope during exertion or stress.
Silent ischemia possible in diabetics and elderly.
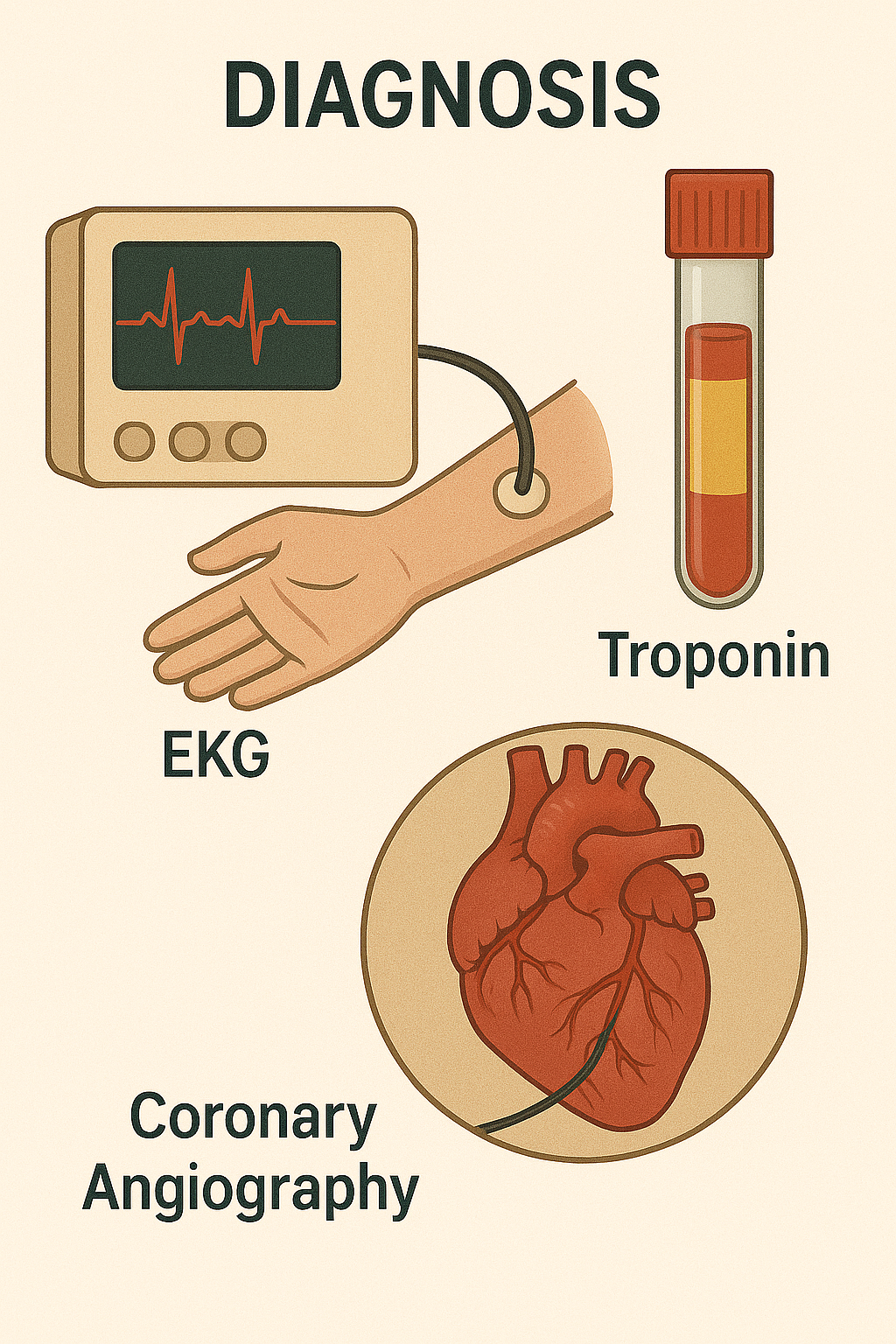
Diagnosis:
ECG: ST-segment depression (stable angina) or elevation (MI).
Cardiac biomarkers: Elevated Troponin I/T in myocardial infarction.
Stress testing for inducible ischemia.
Coronary angiography: gold standard for assessing vessel occlusion.
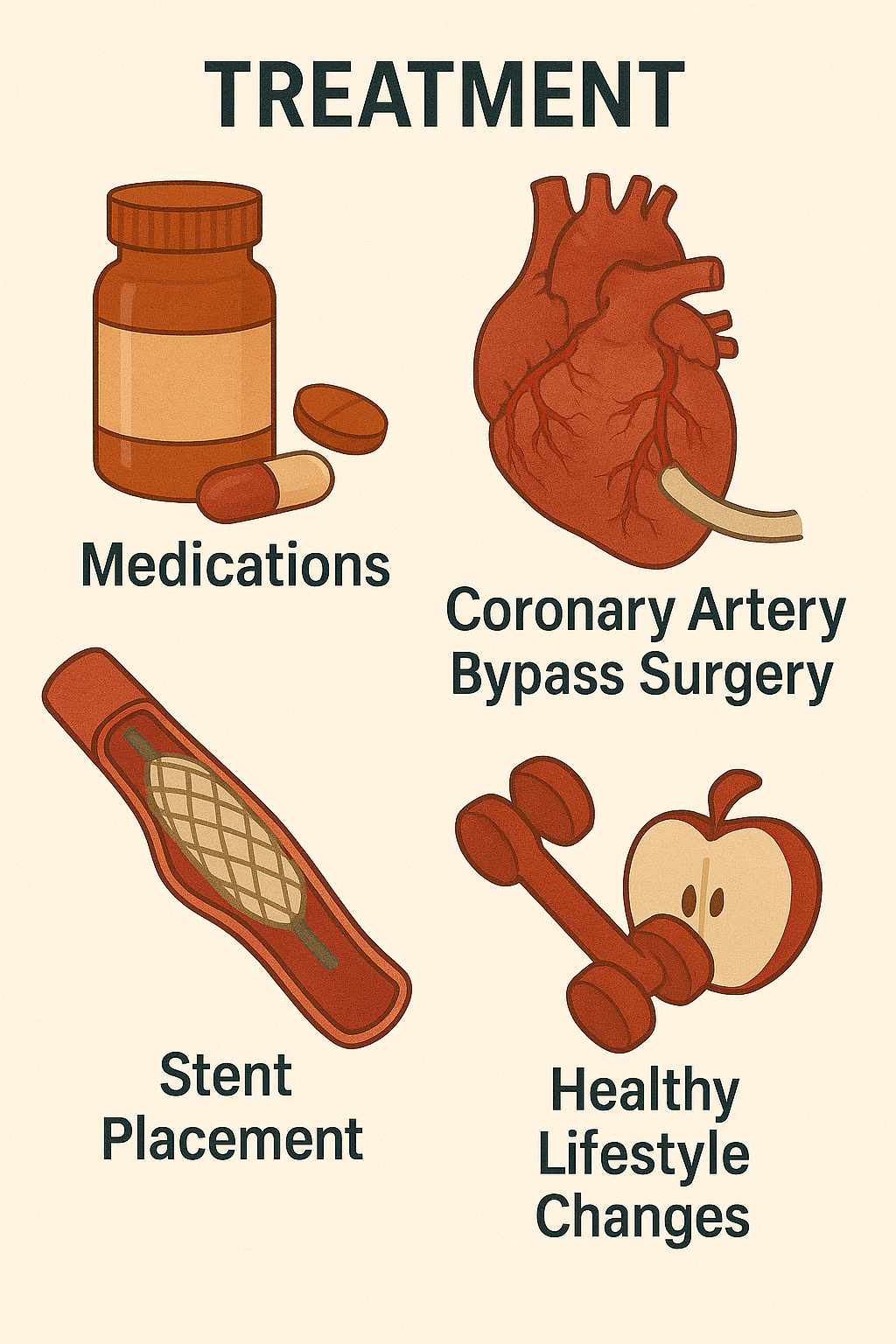
Treatment:
Lifestyle modifications: smoking cessation, exercise, heart-healthy diet, weight control.
Medications:
Antiplatelets (aspirin, clopidogrel)
Statins (reduce LDL, stabilize plaques)
Beta-blockers (lower myocardial O₂ demand)
Nitrates (vasodilation, symptom relief)
ACE inhibitors (improve survival in LV dysfunction)
Procedures:
PCI (stent placement) for localized blockage.
CABG (bypass surgery) for multivessel or left main disease.
-
Add a short summary or a list of helpful resources here.