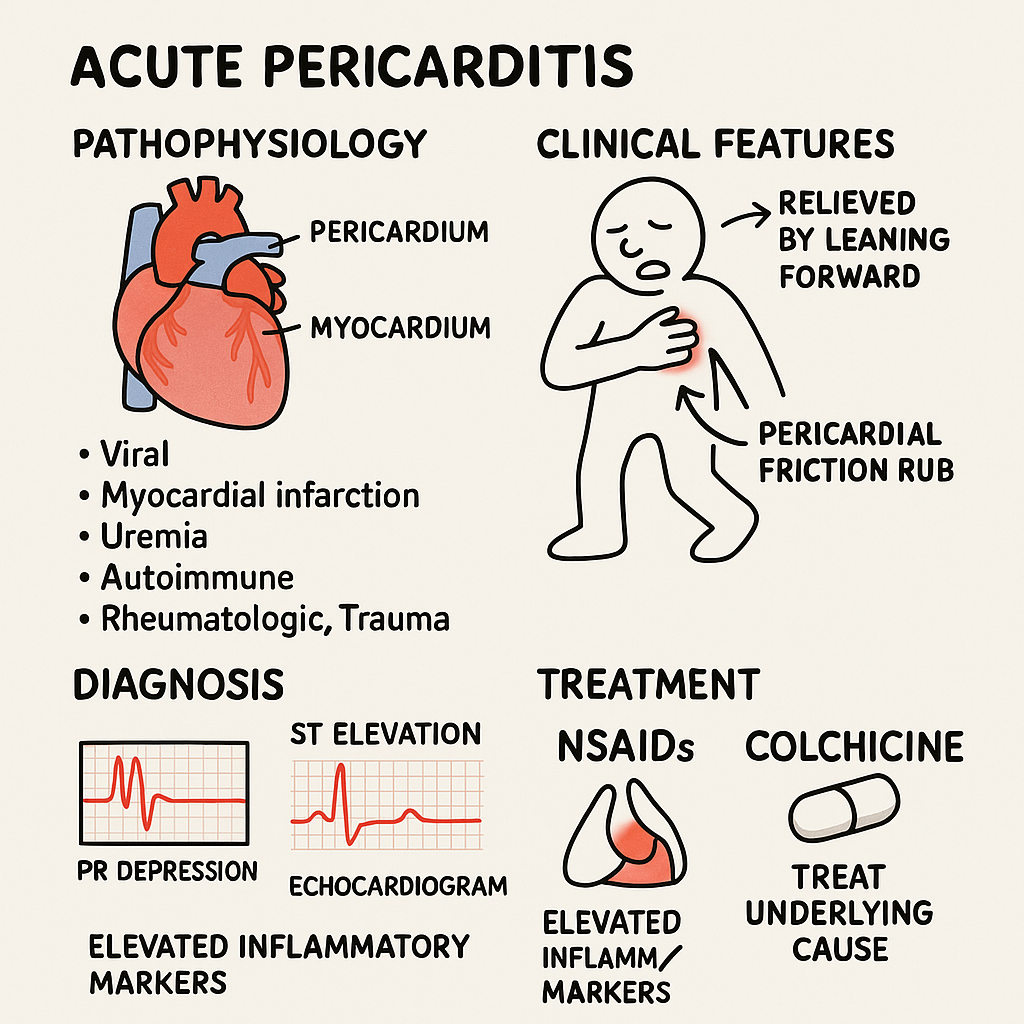
Pathophys
Definition: Inflammation of the pericardial sac (visceral + parietal layers).
Common Causes:
Viral: Coxsackie B (most common)
Post-MI: Early (fibrinous) or Late (Dressler’s syndrome – autoimmune)
Other: Uremia, radiation, connective tissue disease (SLE, RA), trauma, TB.
Mechanism: Inflammatory infiltration → fibrin deposition → pericardial irritation ± effusion.
Clinical Features
Chest Pain: Sharp, pleuritic, relieved by leaning forward, worse on inspiration or lying flat.
Pericardial Friction Rub: Scratchy, triphasic sound best heard at left lower sternal border.
Fever, malaise, tachycardia may occur.
Pulsus paradoxus if tamponade develops.
Diagnosis
ECG Findings (diffuse):
ST-segment elevation (concave, in most leads)
PR-segment depression
T-wave inversion later
Echocardiogram: May show pericardial effusion, rule out tamponade.
Labs: ↑ ESR, CRP; troponin may be mildly elevated (myopericarditis).
CXR: Often normal; may show enlarged cardiac silhouette if large effusion.
Treatment
First-line: NSAIDs (ibuprofen, indomethacin) + Colchicine (reduces recurrence).
Add PPI if on prolonged NSAID therapy.
Steroids: Only if autoimmune or refractory to NSAID/colchicine.
Treat underlying cause:
Dialysis for uremic pericarditis
Antitubercular therapy if TB
Avoid anticoagulation (risk of hemorrhagic effusion).
Monitor for complications:
Pericardial effusion
Cardiac tamponade
Constrictive pericarditis (chronic sequela)