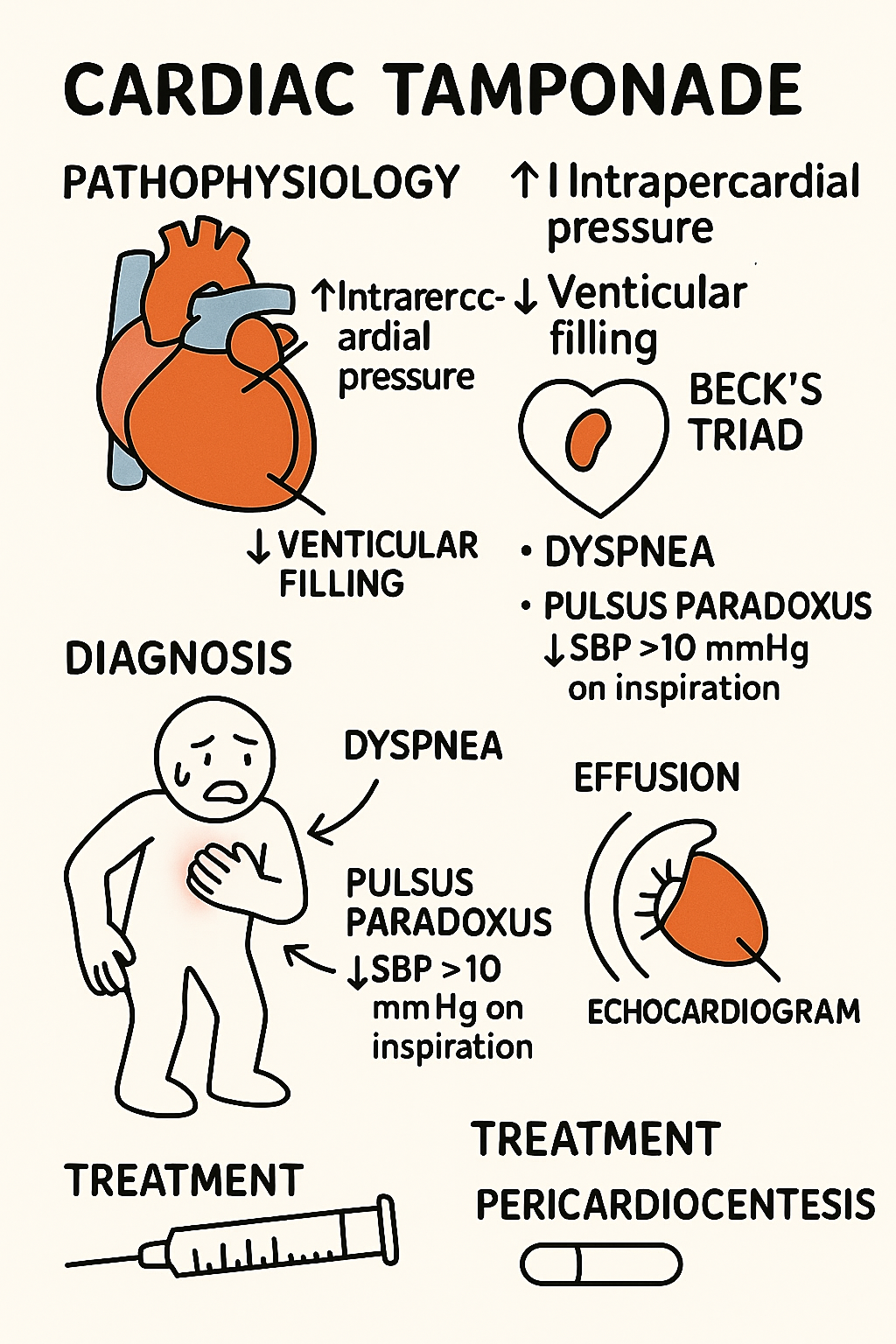
Pathophys
Definition: Life-threatening accumulation of fluid in the pericardial sac causing ↑ intrapericardial pressure → ↓ ventricular filling → ↓ cardiac output.
Mechanism:
Rapid or large pericardial effusion (e.g., trauma, malignancy, uremia).
Equalization of diastolic pressures in all chambers.
Impaired diastolic filling → decreased stroke volume and hypotension.
Clinical Features
Beck’s Triad:
Hypotension – ↓ cardiac output
JVD (Jugular Venous Distension) – impaired venous return
Muffled Heart Sounds – fluid insulation around heart
Additional Findings:
Pulsus paradoxus: ↓ systolic BP >10 mm Hg during inspiration.
Dyspnea, tachycardia, weak pulses
Clear lungs (unlike heart failure)
Diagnosis
Echocardiogram: Pericardial effusion with diastolic collapse of right atrium/ventricle (most sensitive).
ECG: Low voltage QRS, electrical alternans.
CXR: Enlarged, globular heart (if chronic).
Hemodynamics: Equalization of right atrial, pulmonary capillary wedge, and LV diastolic pressures.
Treatment
Pericardiocentesis – definitive treatment.
IV fluids – temporary measure to maintain preload before drainage.
Avoid diuretics (worsen hypotension).
Pericardial window – for recurrent or malignant effusions.