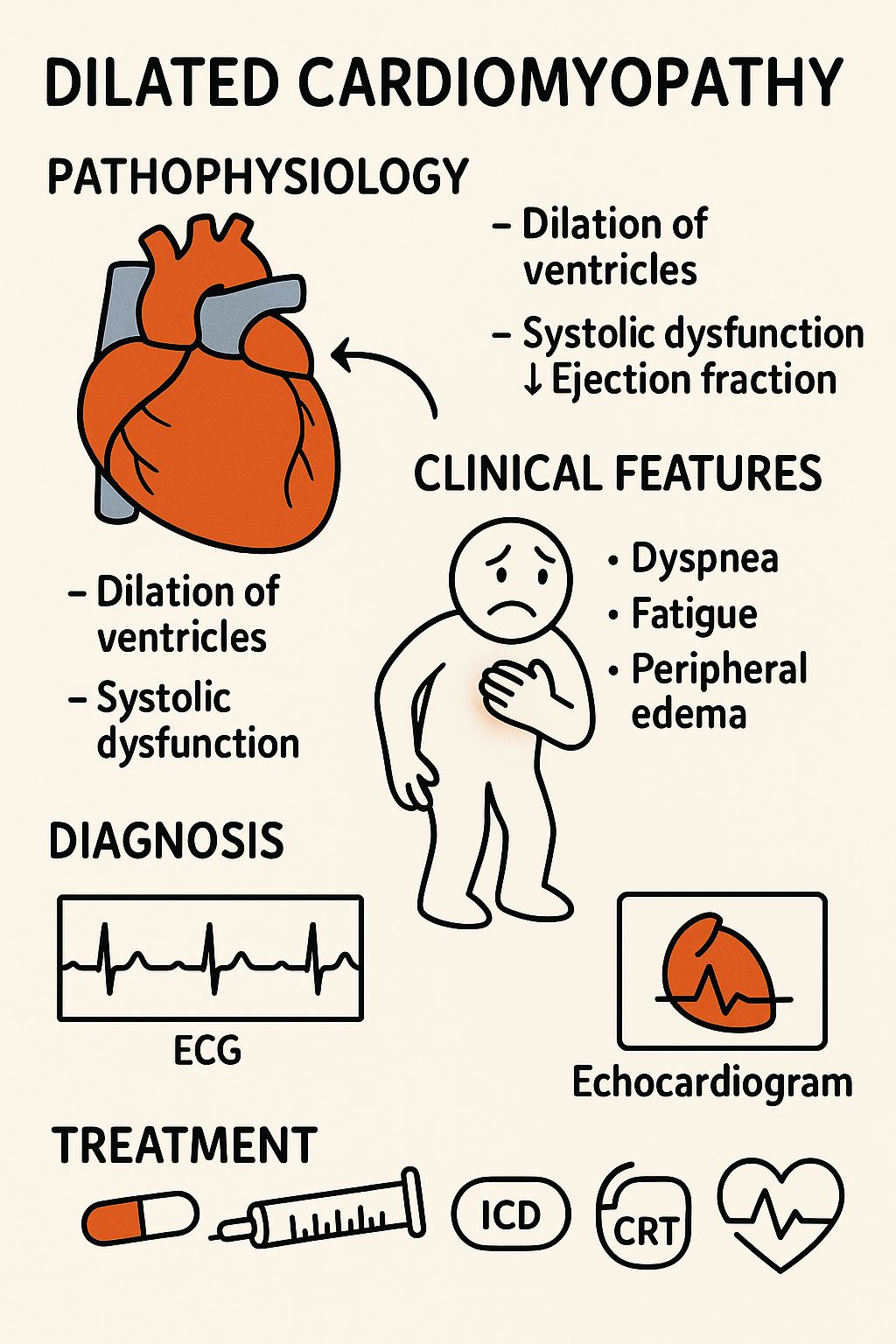
Pathophys
Definition: Dilation and impaired contraction of one or both ventricles → systolic dysfunction (↓ ejection fraction).
Mechanism: Myocyte injury leads to weakening and remodeling of the ventricular wall → ↑ end-diastolic volume, ↓ contractility, and progressive heart failure.
Causes (Mnemonic: ABCCCD):
A – Alcohol abuse (toxic myocarditis)
B – Beriberi (thiamine deficiency)
C – Coxsackie B virus, Chagas disease
C – Cocaine use, Chemotherapy (doxorubicin)
C – Chronic tachycardia or CAD
D – Dystrophies (genetic, Duchenne) / Drugs (doxorubicin)
Clinical Features
Heart failure symptoms:
Dyspnea on exertion, orthopnea, paroxysmal nocturnal dyspnea
Fatigue, exercise intolerance
Signs:
S3 gallop, displaced apical impulse (PMI), crackles, JVD, peripheral edema, ascites
Mural thrombi → risk of embolic stroke or systemic embolism
Diagnosis
Echocardiogram:
Dilated ventricles, ↓ EF (<40%), thin walls, global hypokinesis.
CXR: Cardiomegaly, pulmonary congestion.
ECG: Nonspecific ST-T changes, conduction delay, arrhythmias.
BNP: Elevated.
Coronary angiography: To rule out ischemic cause.
Treatment
Goals: Manage heart failure, prevent complications.
Lifestyle: Sodium and fluid restriction, alcohol cessation.
Medications:
ACE inhibitors / ARBs / ARNIs: ↓ afterload, remodeling.
Beta-blockers: Improve survival.
Diuretics: Symptomatic relief of congestion.
Aldosterone antagonists (spironolactone): ↓ mortality.
Anticoagulation: If mural thrombus or AFib present.
Devices:
ICD: If EF ≤35% (prevention of sudden death).
CRT: If QRS prolonged (>150 ms).
Advanced: LVAD or heart transplant for refractory cases.